Peripheral Arterial Disease (PVD)
The term peripheral arterial disease is widely used to refer to atherosclerotic disease that obstructs the blood supply to the lower limbs (Mohler & Jaff, 2008; NHSUK, 2019).
A major indicator of PAD is intermittent claudication (IC), described below. The reduced blood flow to the limbs can cause the following physical changes:
- The foot may develop dusky erythema as the blood vessels dilate in an attempt to increase blood supply to the tissues that are oxygen deprived
- Hair loss from the limbs
- Diminished or absent foot pulses
- The reduced skin perfusion that can result in inadequate tissue oxygenation, which will promote the development of arterial ulcers of the leg or foot (Vuolo, 2009).

Ischaemic Toe
Ischaemic digital toes in patient with peripheral arterial disease. Ischemia can cause reduced blood flow to the lower limb and consequently poor tissue oxygentation, this then leads to the changes seen. Ischemia is a severe condition that can cause tissue damage and result in loss of limbs. This condition will not improve on its own and requires appropriate medical intervention.
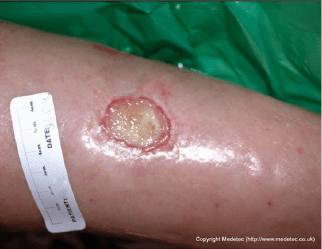
Arterial Leg Ulcer
They develop as the result of damage to the arteries and a lack of blood flow to tissue, PAD. Arterial ulcers are often painful and non-healing ulcers may require urgent treatment is to improve the blood supply.
Intermittent Claudication (IC)
Intermittent claudication is an important indicator of PAD. IC is a symptom related to reduced perfusion through an artery caused by atheroma. During exercise the reduced perfusion causes hypoxia in the muscle distal to the site of atheroma, and a cramping pain is experienced. This pain is relieved by rest. Pain in the calf (the most common area) or foot indicates disease of the femoral or popliteal arteries, and pain in the buttocks and upper thighs indicate disease of the aortoiliac arteries (Vuolo, 2009).
It is important to assess the distance a patient can walk prior to the onset of pain and the ways in which patients find they can relieve the pain. This shows the extent of the patient’s PAD (Vuolo, 2009).
With regular exercise and lifestyle changes, IC symptoms can be resolved (Dealey, 2005). Lifestyle changes will depend upon an individual’s circumstances, but they include smoking cessation, weight reduction, control of hyperlipidaemia, eating a healthy diet and foot care.
However, if PAD progresses, IC pain may become continuous and prevent the patient from sleeping. At this stage, patients find that the symptoms are relieved when their legs are dependant (not elevated). Therefore, they may hang their leg down out of the bed or sleep in a chair to relieve pain. This can progress to chronic critical limb ischaemia (Vuolo, 2009).
Other causes of arterial ulceration include:
- Trauma that interrupts blood flow
- Vasculitis
- Raynaud’s disease
- Cold injuries such as frostbite*
(Vuolo, 2009).
Patients may also develop arterial ulcers due to acute events such as an arterial embolism or severe injury that disrupts blood flow (Moffatt, 2001; Veller, 2011).
*Originally, the cause may be arterial due to hypothermia and peripheral shutdown, but once treated, it rarely continues to be arterial in terms of the underlying cause.