VENOUS LEG ULCERS
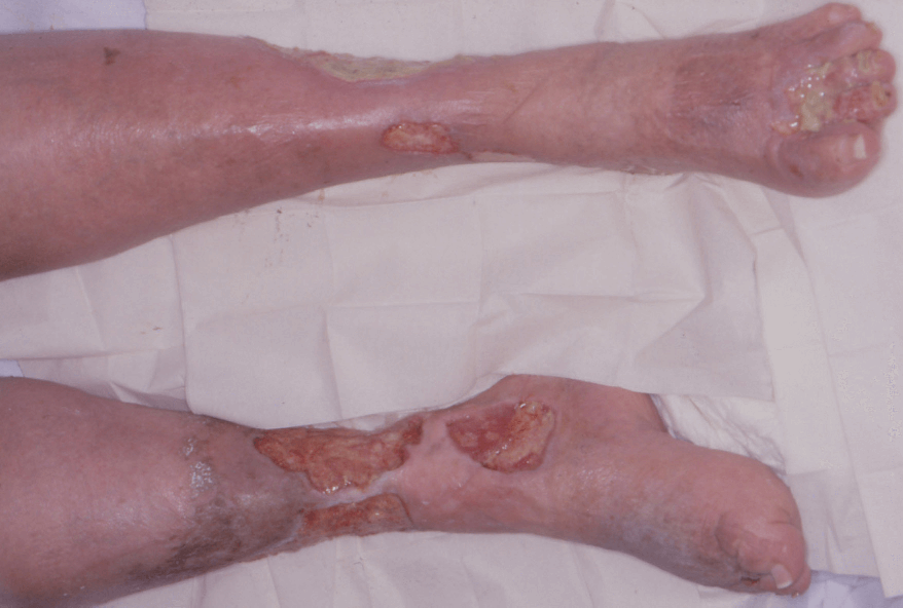
VENOUS LEG ULCERS
A Venous Leg Ulcer (also known as VLU), can be defined as an open lesion between the knee and the ankle joint, which occurs in the presence of venous disease, taking more than two weeks to heal (NICE, 2015; Wounds UK, 2016). Chronic leg ulcer definitions vary. NICE 2015 defines it as “the loss of skin below the knee, leg or foot, which takes more than six weeks to heal”.
It is essential that all VLU’s are diagnosed and then managed as swiftly as possible. Wounds UK Best Practice Statement 2016 recommends that the two-week definition should be used. In patients that have a history of leg ulcers, assessment and treatment of a new lesion should commence as soon as possible.
Venous ulceration is the most common type of leg ulceration (EWMA, 2016). Veins in the lower leg carry blood back to the heart. The venous network comprises of deep veins, which carry blood under high pressure and superficial veins, which are under low pressure. The capillaries, which provide the skin with oxygen and nutrients, then drain into the superficial veins. Small vessels called perforators join the deep and superficial systems (Tortora & Grabowski, 2003).
Veins transport venous blood from the capillaries towards the heart against gravity. There are two factors that ensure that this occurs effectively. Firstly, the calf muscle and, secondly, the valves. This occurs in every vein, but examples here will concentrate on the leg (in relation to leg ulcers).
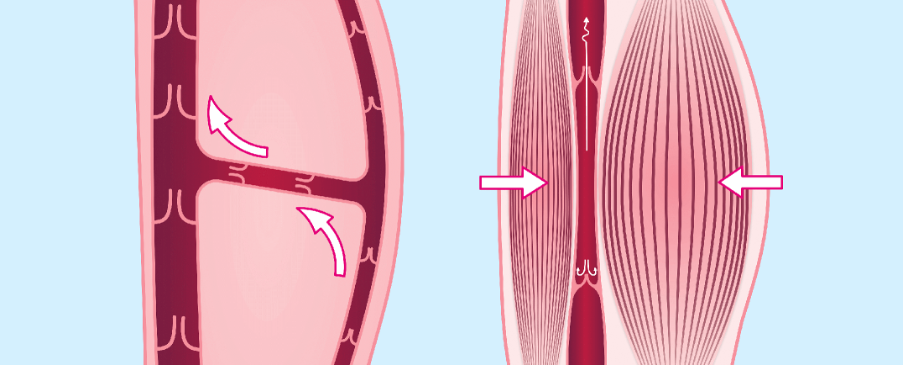
The calf muscle pumps the venous blood through the veins towards the heart. When we exercise our legs, the calf muscles contract and pump the venous blood towards the heart (see image below).
Calf Muscle Pump
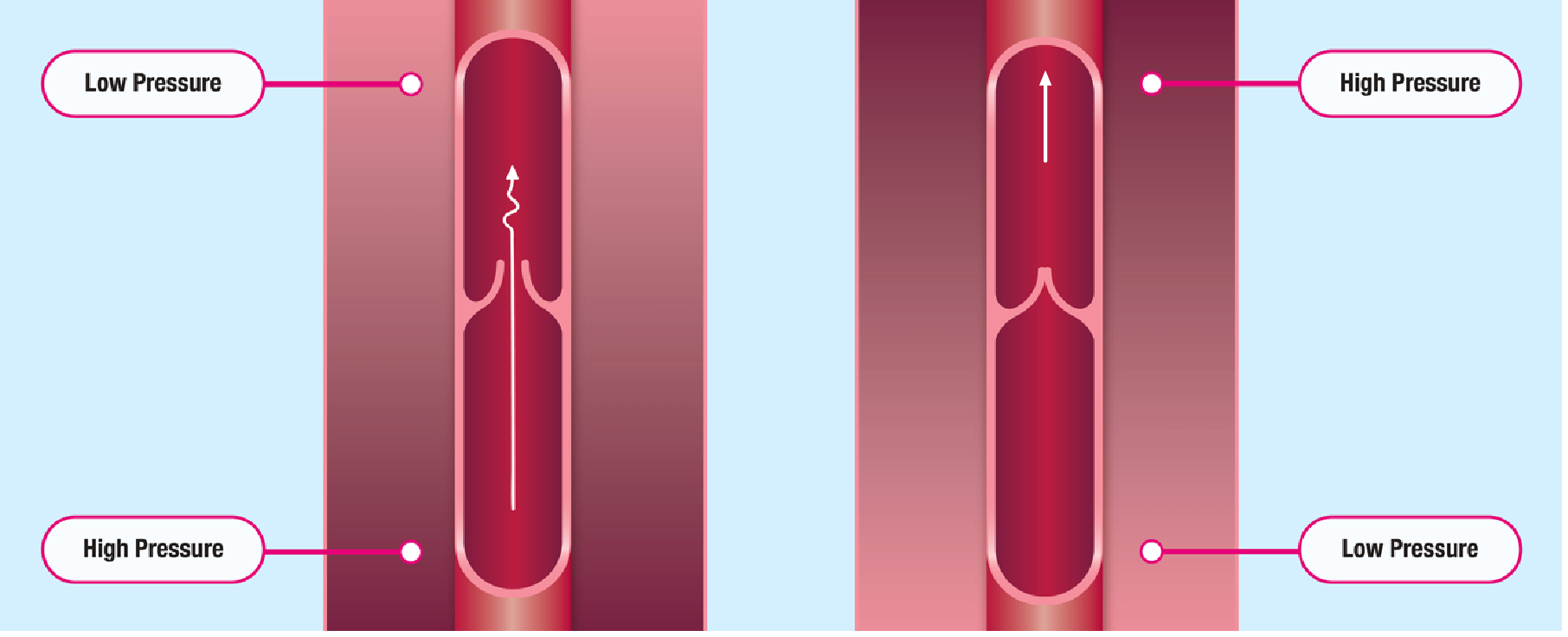
Valves
When blood is pumped up towards the heart, the valves in the veins prevent the blood from running backwards (see image below).
Causes of Venous Leg Ulcers
As shown above, good venous return relies on the effectiveness of both the calf muscle and the valves. Therefore, any disease or injury that affects the calf muscle or venous valves will impede the ability of this mechanism and, ultimately, the health of the leg.
When either of these mechanisms is sufficiently under-performing, blood flow becomes sluggish. This is because there is increased pressure in the veins (venous hypertension), and the body requires a pressure gradient between the arteries and the veins in order for the heart to pump blood through arteries and into veins. Consequently, there is pooling of fluid in the tissues (oedema). The presence of oedema slows down gaseous exchange within the micro-circulation. It also results in reduced tissue oxygenation and inadequate toxin removal (Morison et al., 2004).
Eventually, tissue health suffers, and skin lesions appear with minimal trauma or sometimes without any trauma. Patients are often unaware of the problem until they notice staining on their clothing. The main causes of chronic venous ulcer development are obesity and immobility (Simon et al., 2004; NICE, 2015).
Risk Factors for Venous Ulceration
- Varicose veins
- Deep vein thrombosis
- Chronic venous insufficiency
- Poor calf muscle function
- Arteriovenous fistulae
- Obesity or being overweight
- Mobility issues
- History of leg fracture
- Previous surgery to the leg
- Increasing age
- Chronic oedema
- Family history
- History of intravenous drug use
(Wounds UK BPS, 2016)